Diabetic foot
Varicose Veins
Piles
Fissure
Fistula
Pilonidal sinus
Circumcision
Hernia
Hydrocele
Hysterectomy
Gynaecomastia
Lipoma
Sebaceous cyst
Diabetes
Diabetic foot
Gastric ulcer
Appendicitis
Thyroid surgery
Burns
Trauma & Accident care
Intestinal perforation
Intestinal obstruction
DVT
Gallstone
Metabolic and Bariatric
Quality Care for Diabetic Foot Conditions in Rajahmundry
What is Diabetic foot
Diabetes is a chronic medical condition characterized by high levels of sugar (glucose) in the blood. The condition occurs when the pancreas is unable to produce enough insulin (Type 1 diabetes) or the body cannot effectively use the insulin it produces (Type 2 diabetes). Insulin is a hormone that regulates blood sugar levels, and when it is not functioning properly, it can lead to a buildup of glucose in the blood. Over time, high blood sugar levels can cause damage to the blood vessels, nerves, and organs in the body, leading to a range of complications.
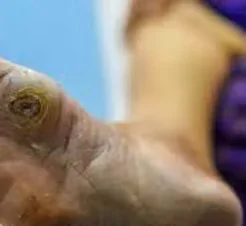
Symptoms of Diabetic foot
The symptoms of diabetic foot can vary depending on the severity of the condition. Some common symptoms include:
Numbness or tingling in the feet
Burning or shooting pain in the feet or legs
Swelling in the feet or ankles
Changes in the color or temperature of the skin on the feet
Open sores or ulcers that are slow to heal
Ingrown toenails or other foot deformities
Dry, cracked skin on the feet or toes
Fungal infections such as athlete’s foot
Increased foot odor
Difficulty walking or balancing.
It is important to seek medical attention if you experience any of these symptoms, as prompt treatment can help prevent serious complications.a
Causes of Diabetic foot
Diabetic foot is caused by a combination of factors related to diabetes, including:
Nerve damage (neuropathy): High blood sugar levels over time can damage the nerves in the feet, which can lead to loss of sensation and an inability to feel pain, heat, or cold.
Poor blood circulation: Diabetes can cause damage to blood vessels, which can impair blood flow to the feet and legs, making it more difficult for wounds to heal.
Compromised immune system: Diabetes can weaken the body’s immune system, making it more difficult to fight infections.
Foot abnormalities: Diabetes can cause foot deformities, such as hammertoes or bunions, that can increase the risk of developing pressure points and ulcers on the feet.
Poor foot care: Poor foot hygiene and ill-fitting shoes can increase the risk of developing foot problems in people with diabetes.
Other health conditions: People with diabetes who have other health conditions such as peripheral artery disease or kidney disease are at increased risk of developing diabetic foot.
Proper management of blood sugar levels and regular foot care can help reduce the risk of developing diabetic foot.
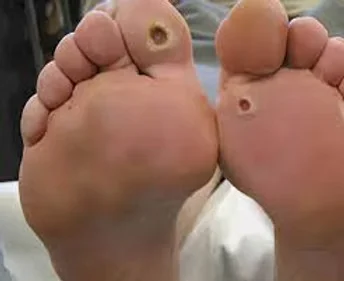
Treatment
Blood sugar control: Maintaining tight control of blood sugar levels can help prevent further nerve damage and improve circulation.
Wound care: Proper wound care is essential to prevent infection and promote healing. This may include cleaning the wound, applying topical medications, and changing dressings regularly.
Antibiotics: If an infection is present, antibiotics may be necessary to help fight the infection.
Offloading: Pressure relief is crucial for diabetic foot ulcers to heal. This can be achieved through offloading techniques such as using special shoes, casts, or braces.
Surgery: In some cases, surgical intervention may be necessary to remove dead tissue or correct foot deformities that are contributing to the problem.
Education and prevention: Education on proper foot care, including daily foot inspections and regular checkups with a healthcare provider, can help prevent the development of diabetic foot complications.
It is important to seek medical attention promptly if you have any symptoms of diabetic foot, as early treatment can help prevent serious complications

FAQs around Diabetic foot
What are the symptoms of diabetic foot?
There are several risk factors that can increase the likelihood of developing diabetes, including family history, being overweight or obese, leading a sedentary lifestyle, having high blood pressure or high cholesterol, and certain medical conditions or medications. .
How is diabetic foot diagnosed?
While some risk factors for diabetes, such as family history and age, cannot be changed, other risk factors can be managed or prevented through healthy lifestyle choices such as regular exercise, maintaining a healthy weight, eating a balanced diet, and avoiding smoking and excessive alcohol consumption.
How can diabetic foot be prevented?
Diabetes can be diagnosed through a blood test that measures blood sugar levels. Additional tests may be ordered to determine the type of diabetes and assess for any complications.
Are there any complications associated with diabetic foot?
Uncontrolled diabetes can lead to several complications over time, including damage to the eyes, kidneys, nerves, and blood vessels. It can also increase the risk of heart disease and stroke. Proper management of diabetes, including blood sugar control and regular medical checkups, can help prevent or manage these complications.
Get in Touch
For any questions fill out our form

Make
Appointment
&
Take Care Of Your
Healthy Life
